Why Is My Vision Fluctuating with Diabetes?
Living with diabetes requires constant vigilance. Between monitoring glucose levels, managing diet, and keeping up with medication, there is a lot to juggle. However, one of the most unsettling symptoms many patients report isn’t found on a finger-prick test—it’s in their line of sight.
If you have noticed that your vision seems clear one hour and blurry the next, you are experiencing fluctuating vision diabetes patients often describe as a "rollercoaster for the eyes." At Eyes & Eyelids, we understand how distressing this can be.
In this guide, we will explore why blood sugar causes these shifts, how to distinguish temporary changes from permanent damage, and what you can do to stabilise your sight.
The Science: Why Does Blood Sugar Affect My Sight?
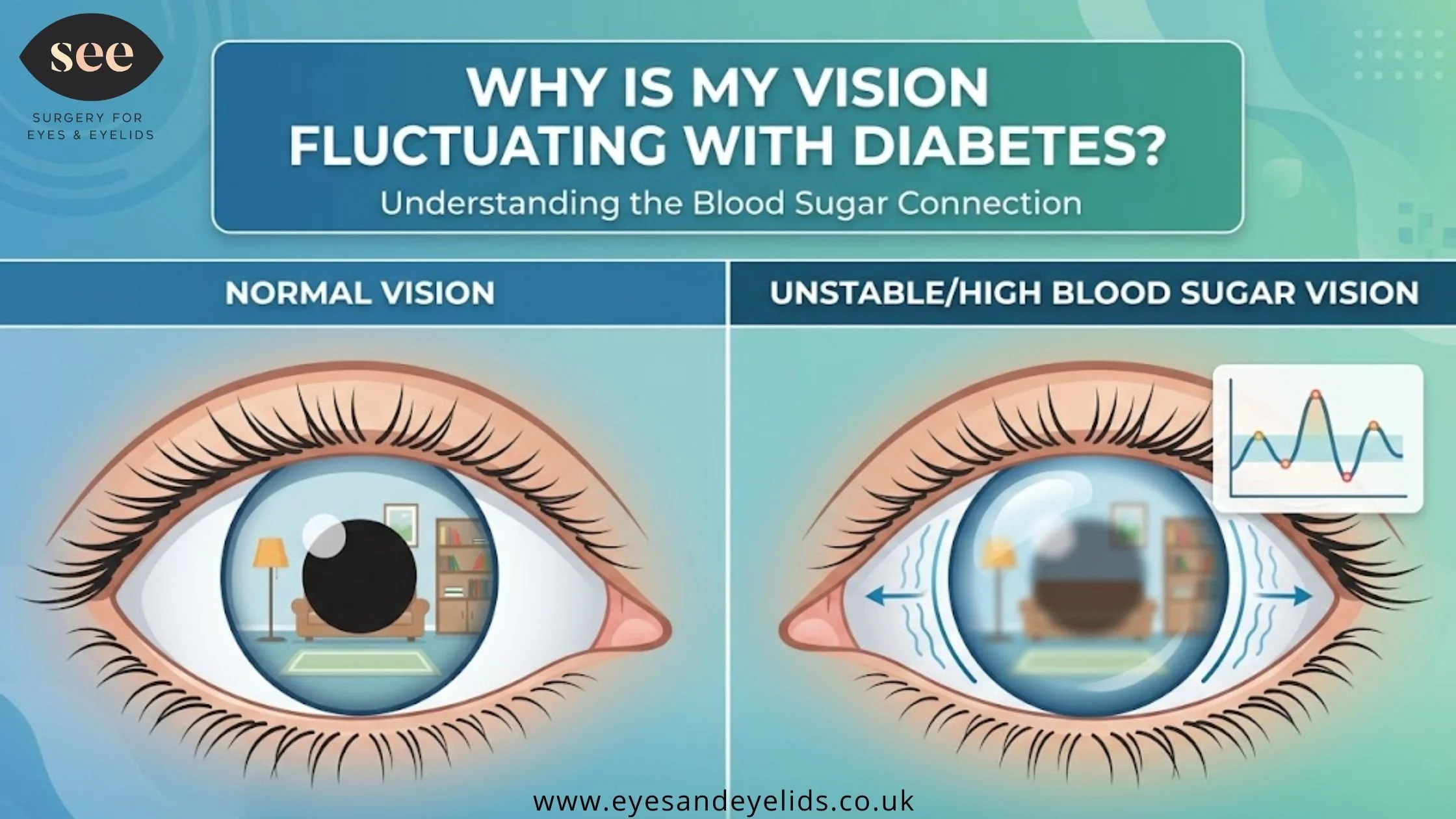
To understand why your vision changes, we have to look at the anatomy of the eye—specifically the crystalline lens. The lens is a clear, flexible structure responsible for focusing light onto the retina.
When your blood sugar (glucose) levels are high, the excess sugar spills over into the fluids surrounding the eye. Through a process called osmosis, the lens absorbs this extra glucose and water, causing it to swell and change shape.
Because the lens is now a different shape, its ability to refract light is altered. This results in blurry vision diabetes causes temporarily. When your sugar levels drop back down to a normal range, the water leaves the lens, it shrinks back to its original size, and your focus returns. This "accordion effect" is the primary reason for those frustrating daily fluctuations.
Fluctuating Vision vs. Diabetic Retinopathy: Knowing the Difference
It is vital for patients to distinguish between temporary refractive changes and the more serious, long-term condition known as diabetic retinopathy.
1. Temporary Blood Sugar Vision Changes
These usually occur when your glucose levels are poorly controlled or when you are starting a new treatment plan.
The Feeling: Vision feels "out of focus" or "smudged."
The Pattern: It changes throughout the day or improves as your HbA1c levels stabilise.
The Risk: Generally low, provided sugar levels are brought under control.
2. Diabetic Retinopathy Symptoms
This is a complication where high blood sugar damages the tiny blood vessels in the retina (the back of the eye).
The Feeling: Seeing "floaters" (dark spots or cobwebs), shadows, or "blank spots" in your vision.
The Pattern: These changes are often permanent and do not fluctuate based on your hourly sugar readings.
The Risk: High. If left untreated, it can lead to permanent sight loss.
Why Is My Vision Blurry After Starting Insulin?
A common point of confusion for many patients occurs shortly after they begin a new insulin regimen or intensive glucose management. You might expect your vision to improve as your numbers get better, but often, the opposite happens: your vision becomes significantly blurrier.
This is known as insulin-induced blurred vision. As your blood sugar drops toward a healthy range, the fluid balance in your eyes shifts rapidly. It can take several weeks (sometimes up to six weeks) for the lens of the eye to "recalibrate" to these lower glucose levels.
Our Advice: Do not rush to the optician for a new prescription during this transition period. Your vision is in flux, and any glasses made now will likely be incorrect once your levels stabilise.
When Should I See an Ophthalmologist?
While daily fluctuations are often related to glucose levels, you should never self-diagnose. In the UK, the NHS Diabetic Eye Screening Programme is essential, but if you notice any of the following "red flag" symptoms, you should book an appointment with a specialist at Eyes & Eyelids immediately:
Sudden loss of vision in one or both eyes.
Flashers and Floaters: Seeing sudden flashes of light or a shower of new dark spots.
Distorted lines: Straight lines (like door frames) appearing wavy or bent.
A "curtain" effect: A dark shadow spreading across your field of vision.
These can be signs of advanced diabetic retinopathy or a retinal detachment, both of which require urgent clinical intervention.
Practical Steps to Stabilise Your Vision
Managing blood sugar vision changes is a marathon, not a sprint. Here is how you can protect your eyes and reduce the frequency of fluctuations:
1. The "Golden Rule" of Stability
Avoid "spiking." Large swings between very high and very low glucose are more damaging to the blood vessels in the eye than a steady, slightly elevated level. Use continuous glucose monitors (CGM) if available to track your trends.
2. Stay Hydrated
Dehydration can affect the fluid pressure within your eyes. Drinking plenty of water helps your body manage glucose more efficiently and supports overall ocular health.
3. Record Your "Vision Log"
If you notice your vision is particularly bad at certain times of the day, note down your blood sugar reading at that moment. Sharing this log with your ophthalmologist or GP can help them determine if your symptoms are purely refractive or symptomatic of underlying damage.
4. Blood Pressure and Cholesterol
Diabetes rarely acts alone. High blood pressure (hypertension) puts extra strain on the delicate vessels in your retina. Managing your "ABC" (A1c, Blood Pressure, and Cholesterol) is the most effective way to prevent diabetic eye disease.
Treatment Options at Eyes & Eyelids
If your fluctuating vision is found to be a symptom of underlying diabetic retinopathy or Macular Oedema (swelling of the central retina), modern medicine offers highly effective treatments.
Intravitreal Injections: Medications (Anti-VEGF) that help reduce swelling and stop the growth of abnormal blood vessels.
Laser Therapy: Used to seal leaking blood vessels and prevent further vision loss.
Advanced Surgery: For complex cases involving vitreous haemorrhage or retinal scarring.
At Eyes & Eyelids, led by our specialist consultants, we use state-of-the-art diagnostic tools like Optical Coherence Tomography (OCT) to see beneath the surface of your retina and catch problems before they affect your sight permanently.
Summary: Clarity Through Control
Fluctuating vision is your body’s way of telling you that your glucose levels are on a journey. While it is a common symptom of diabetes, it should always be the catalyst for a check-up.
By maintaining a stable blood sugar range and attending regular eye screenings, you can stop the "rollercoaster" and ensure your vision remains clear for years to come.
Are you concerned about your vision? Don't wait for your next annual screening. Contact the experts at Eyes & Eyelids today for a comprehensive diabetic eye assessment.
Book a Consultation at Eyes & Eyelids
Frequently Asked Questions (FAQs)
-
In most cases, if the blurriness is caused by lens swelling due to high glucose, your vision should begin to clear within two to six weeks after your blood sugar levels have returned to a consistent, healthy range. It is important to be patient during this "settling" period, as the fluid balance in the eye takes time to recalibrate.
-
Diabetes typically causes "blurring" rather than total blindness. However, extremely high blood sugar can cause vision to become so distorted that it feels like significant sight loss. Furthermore, a sudden "blackout" or curtain-like shadow in your vision could indicate a vitreous haemorrhage or retinal detachment—both are medical emergencies and require immediate attention.
-
No. We strongly advise against purchasing a new prescription while your blood sugar is poorly controlled or if you have just started a new insulin regimen. Because the shape of your lens is changing, any prescription you get today will likely be incorrect once your levels stabilise, resulting in a waste of money and continued eye strain.
-
Not necessarily. Blurry vision is often just a temporary refractive change caused by blood sugar vision changes. However, because blurriness is also a secondary symptom of diabetic retinopathy, the only way to be certain is through a dilated eye exam and OCT scanning at a specialist clinic like Eyes & Eyelids.
-
Many diabetic patients find their vision is cloudier in the morning. This can be due to glucose fluctuations overnight or "dry eye syndrome," which is significantly more common in people with diabetes. If your glucose was high before bed, your lens may still be swollen when you wake up.